Surgical Removal of Skin Cancer in Sydney by Plastic Surgeons
Melanoma is one of the most dangerous types of skin cancer that can form in different skin areas of your body including the face, neck, arms, legs, and back.
A skin growth or a mole could be a Melanoma if it’s asymmetric, unevenly coloured, or has an irregular border with the skin surrounding it. If in any doubt, get a medical practitioner to check it as soon as possible.
The surgical removal of melanoma skin cancer can be done with a “wide local excision” surgery for patients in the early stages. This involves taking 1 – 2 cm perimeter around the area and a suitable depth beneath it. Each melanoma is individually assessed and the risk of spread to nearby lymph nodes calculated. For many patient the first lymph node downstream of the melanoma needs to be sampled. This is call a sentinel lymph node biopsy and it helps to assess the overall risk and danger. This in turn allows the team to work out the best treatment options which may be nothing further, medical treatments such as immunotherapy and targeted therapy or sometimes further surgery, radiation therapy, or chemotherapy.
Sydney Specialist Plastic Surgeons Dr Varun Harish, Dr Hari Alani and Dr Michael Kernohan are highly trained surgeons performing skin cancer surgery. They have experience using advanced surgical approaches and reconstructive skin techniques to remove melanoma tumours, especially those in cosmetically challenging or highly functional areas such as the face, palms, and soles of the feet.
The Pure Visage Plastic Surgery Clinic is located in Gregory Hills.
What Is Melanoma?

Melanoma is a serious form of skin cancer that begins in melanocytes – skin cells that produce melanin (the pigment that gives your skin its colour). When these skin cells have DNA damage, new cells start to grow out of control until they form a mass of cancerous cells.
Exposure to UV (ultraviolet) radiation from the sun and from tanning lamps and beds is thought to be the leading cause of melanoma since melanoma usually develops in the areas of the body most exposed to the sun. These areas include your Back, Legs, Arms, Neck and Face.
Scientists believe that the DNA damage is likely due to a combination of environmental and genetic factors because melanoma skin cancer can also occur in areas that don’t receive a lot of sun exposure. They can be seen in people with darker skin and occur in places most people wouldn’t think to check, such as:
- The spaces between your toes
- Your palms
- Soles of your feet
- Your scalp
- The genitals
- Inside your mouth
The first signs and symptoms of melanoma usually begin as:
- Changes in an existing mole
- The appearance of a pigmented or unusual-looking growth on your skin
Melanoma can be confined to the upper layer of the skin and is usually treatable with surgery. Sometimes, melanoma skin cancer can metastasize to nearby lymph nodes or other organs of the body becoming more dangerous and more challenging to treat.
Look for Suspicious Features – Signs of Melanoma
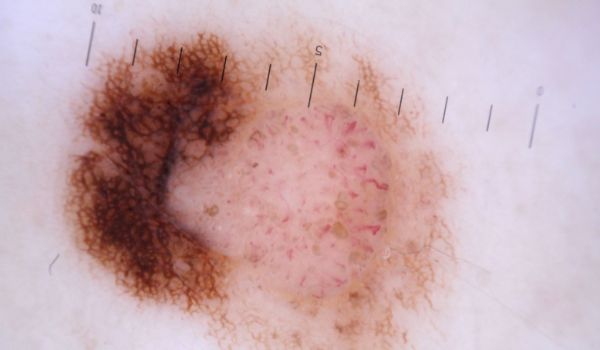
Most moles appear during childhood but you can continue getting new moles until the age of 40. An adult has between 10 and 40 moles on average that can change appearance over time or disappear with age.
Regular moles usually:
- Have a tan, brown, or black colour
- Have an oval or round shape
- Are smaller than 6 mm in diameter (the size of a pencil eraser)
Regular moles have a uniform colour with a defined distinct border separating them from the skin surrounding them. A mole may indicate melanoma when it starts showing the following suspicious characteristics:
- An asymmetrical shape with two different-looking halves
- An irregular or notched border
- Changes in colour- the mole may have more than one colour or a non-uniform colour distribution
- A diameter that is larger than 6 mm
- The mole may also become itchy or start bleeding
Cancerous or malignant moles can differ a lot in appearance. Some melanoma moles may have all the irregular changes while others may have only one or two unusual characteristics.
Make an appointment with your skin doctor or dermatologist when you notice any skin changes that might seem unusual or concerning.
Download Dr Michael Kernohan’s Cost of Plastic Surgery Guide
Surgery for Melanoma Skin Cancer
The best options for melanoma treatment option will depend on how much the melanoma has spread and the location of the skin lesion. Surgery to remove the tumour is almost always the best way to treat early-stage melanoma.
On the other hand, more advanced melanomas that have spread beyond the original lesion can be more difficult to treat. Metastatic melanoma may need additional treatment before or after melanoma resection surgery by a surgeon. Your Melanoma surgery options can include:
1. Melanoma Excision Surgery
Early-stage melanoma tumours that haven’t spread beyond the upper layers of the skin are usually successfully treated by melanoma excision surgery alone.
Dr Michael Kernohan uses surgical reconstructive techniques to repair the area affected by melanoma and give you the best cosmetic outcome possible after the melanoma is removed.
Before removing the skin lesion, Dr Kernohan will carefully consider:
- The thickness of the tumour
- The location of the tumour
- How removing the tumour might affect your function and cosmetic appearance
During melanoma resection surgery, Dr Kernohan will perform the following:
- The first step is a skin biopsy – this is often done by the GP or dermatologist. Once part or all of the skin lesion has been removed it is sent to a lab for analysis and diagnosis. Very thin melanoma may be completely removed during the biopsy and occasionally require no further treatment
- After that, he will use a scalpel to remove 1-2cm perimeter around and a suitable depth underneath the area to remove any stray melanoma cells. While doing so, Dr Kernohan pays attention to the amount of tissue removed and preserving the appearance of your skin while making sure all of the cancer is removed
- Dr Kernohan will also deliberately remove some of the healthy tissue from around the tumour to make sure no cancer cells are left behind
- The wound will be reconstructed to leave as little trace as possible. This is an especially important and challenging step when the melanoma is on the face, specifically near the nose, eyes, or lips. Removing a skin lesions in this area requires significant surgical skills to prevent any deformities and reconstruct the affected area
- Finally, the wound will be often closed with plastic surgery techniques to reduce the visible appearance of scarring.
- After the surgery, the margins of the resected skin are checked to make sure they are cancer-free. If they are, often no further surgery will be required

2. Lymph Node Biopsy
This type of biopsy focuses on the first lymph node where the tissue fluid(lymph) drains to – this is called a sentinel node biopsy. Sentinel lymph node is the first one to trap stray cancerous cells – from this point the cancer spreads in the lymphatic system. Removing the sentinel lymph node can determine if the tumour has affected the lymphatic system. A negative result of the biopsy suggests a better prognosis and a positive lymph node often leads to further tests and advanvced medical treatments.
3. Metastatic Melanoma Surgery
Advanced melanoma that has spread from the skin to other organs such as the lungs, liver, or brain can be more difficult to treat.
The treatment of metastatic melanoma can require surgery with additional treatment before or after surgery to shrink the tumour and slow down the disease. Treatment plans are tailored to the individual by a multidisciplinary team of Doctors.
Patients with metastatic cancer have options for supplemental or adjuvant treatments that aim to increase the effectiveness of skin cancer surgery and survival. These additional treatments include:
- Immunotherapy: This is a type of drug therapy that helps your immune system in fighting cancer. Immunotherapy is usually recommended after melanoma surgery for skin cancer that has spread to the lymph nodes or other areas of the body
- Targeted therapy: Targeted drug treatments focus on weaknesses within the cancer cells. By targeting these weak points, the drugs are able to kill skin tumor cells
- Radiation therapy: High-powered energy beams such as X Rays and protons are used to kill melanoma cancer cells. These beams may be directed to the lymph nodes if cancer has spread there. It can also be used to treat melanoma that cannot be completely removed with excision surgery
- Chemotherapy: Chemotherapy uses drugs that are given intravenously (IV), in pill form, or both to kill skin cancer cells
How Is Melanoma Diagnosed?
When you spot a suspicious mole or irregular skin tissue, your healthcare provider will perform the following to confirm a skin melanoma diagnosis:
- Physical exam: After giving your health history, your skin will be examined for irregularities and specific signs of melanoma
- Biopsy: A sample of the suspicious skin tissue is removed and sent to a lab where a pathologist determines whether it has cancer cells
After cancer is confirmed and the type of melanoma is determined, your medical team will identify the stage of your melanoma. The stage is determined by how much cancer has grown and whether it metastasized (spread).
Knowing the stage of melanoma is crucial and helps decide how to best treat the disease. The staging process is based on three factors:
- Thickness: The thickness of the tumor, also known as Breslow thickness or Breslow depth, is an important factor in predicting how far the melanoma has advanced. The thinner the Breslow thickness, the less likely the tumor has spread
- Ulceration: Tumor ulceration is the breakdown of skin on top of the skin lesion. Melanomas with ulceration are more serious and have a greater risk of spreading than those without ulceration
- Spreading: The stage of melanoma is also determined by whether cancer has already spread to nearby or distant lymph nodes and other organs such as the lungs and the brain
Identifying the stage of the melanoma disease may require additional blood tests or imaging techniques such as a PET scan, CT scan, or MRI.
The diagnosis and treatment of melanoma can require a multidisciplinary effort. Your Plastic Surgeon can coordinate with dermatological specialists, oncologists, and imaging doctors to find the right treatment plan for you with the best cosmetic outcomes.
As an experienced plastic surgeon, Dr Kernohan is able to remove challenging melanoma tumors and lesions lowering both the functional and cosmetic impacts. He meticulously hides the incisions within the folds of the skin and performs reconstructive surgery.
Further Reading about Skin Cancer Procedures
- Read the BCC Skin Cancer Surgery Page
- Read the SCC Squamous Cell Carcinoma Surgery
- Read the Blog Is it Melanoma or Skin Cancer? – Be Sunsafe



 Dr Varun Harish FRACS (Plas) – Plastic Surgeon
Dr Varun Harish FRACS (Plas) – Plastic Surgeon




